Studio Partner 3 a 2 anni
New trial data shows SAPIEN 3 TAVI continues to meet the needs of patients with sAS
Your sAS patients are still in urgent need of treatment. They need a procedure with optimal clinical outcomes, fewer complications and a quick return home. The 2-year results from the PARTNER 3 Trial continue to show favourable outcomes of SAPIEN 3 TAVI compared to surgery.
SAPIEN 3 TAVI has demonstrated proven benefits in low-risk patients
Results from the PARTNER 3 Trial in low-risk patients demonstrated the superiority of SAPIEN 3 TAVI vs. surgery for the primary composite endpoint of death, stroke, or rehospitalization at 1 year – opening‡ up new treatment options for low-risk patients with sAS.¹
The recently reported 2-year results of the PARTNER 3 Trial underline the 1-year superiority of SAPIEN 3 TAVI vs. surgery, meaning patients can benefit from better outcomes as well as shorter hospital stays, to help them get back to their lives sooner.1,2
PARTNER 3 Trial overview
Baseline characteristics and trial design1,2
- Mean age: 73 years
- Mean STS score: 1.9
- Mean no. of NYHA class III or IV: 132
- 1000 low-risk patients with sAS
- 1:1 randomization to undergo SAPIEN 3 TAVI or surgery
Primary endpoint1,2
- Composite of all-cause mortality, stroke, or rehospitalization at 1 year post-procedure
Key results after 1 year of follow-up
SAPIEN 3 TAVI demonstrated superiority over surgery, with a 46% reduction in the composite primary endpoint of all-cause mortality, all stroke and rehospitalization, from 15.1% in the surgical group to 8.5% with TAVI (HR 0.54; 95% CI, 0.37 to 0.79; P=0.001).2
Quality of life also improved, with a significantly higher KCCQ overall summary score recorded with TAVI vs. surgery.*3
A continued significant benefit in the composite primary endpoint after 2 years
The latest results in the composite primary endpoint confirm that even after two years, patients can benefit from positive outcomes compared to surgery and are less likely to be rehospitalized.1
Highlights from the 2-year data review
SAPIEN 3 TAVI resulted in a 37% risk reduction in the primary endpoint of all-cause death, all stroke and rehospitalization (P=0.007), as shown in Figure 1.1
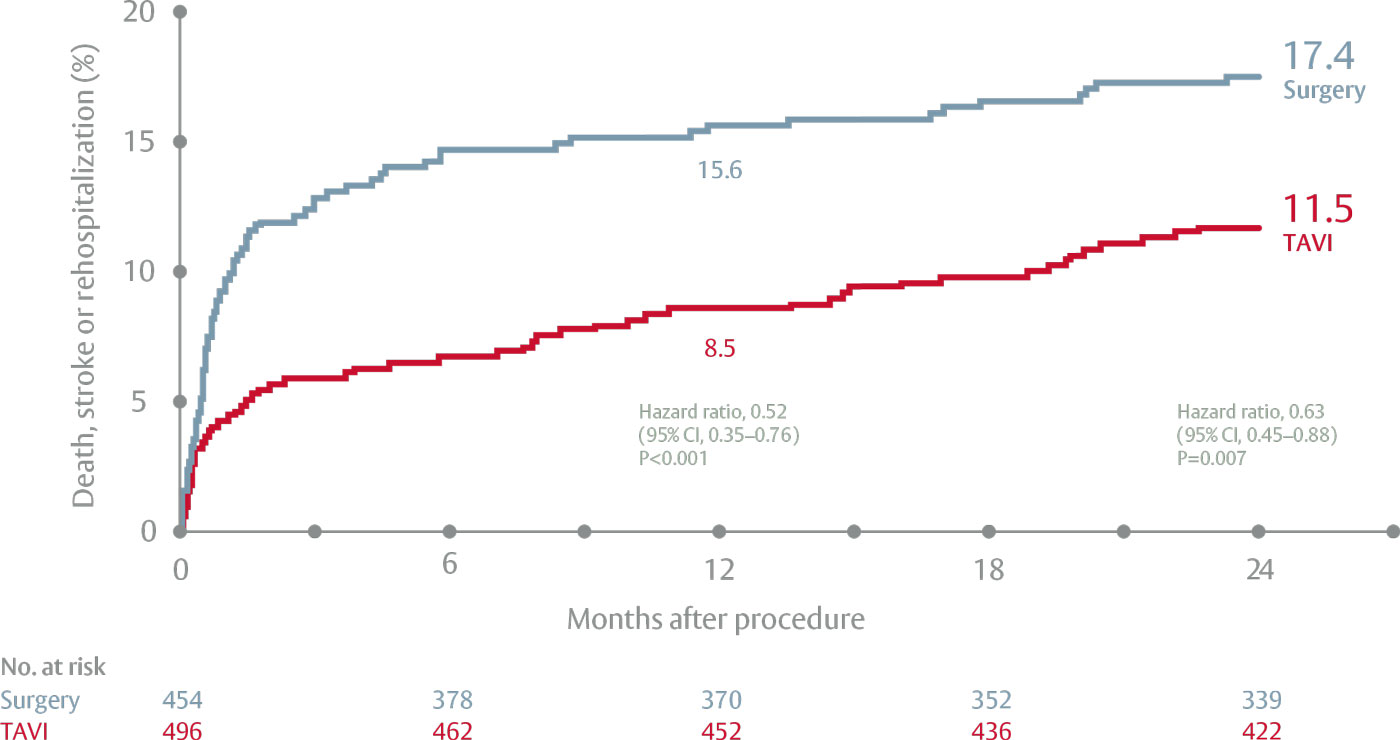
Figure 1 – Primary composite endpoint of all-cause death, all stroke and rehospitalization.1
A significant reduction in rehospitalization was also seen in the TAVI arm vs. surgery (P=0.04).1
Additional results
In addition, results after 2 years of follow-up showed:
- A trend towards lower rates of death and stroke at 2 years with TAVI vs. surgery (no statistical significance)1
- Improvements in mean gradient were sustained from 1 to 2 years of follow-up1
- The frequency of moderate or mild paravalvular regurgitation remained unchanged between 1 and 2 years of follow-up1
Guide your sAS patients to a fast and low-risk treatment – refer them for TAVI evaluation
The benefits of SAPIEN 3 TAVI shown in the PARTNER 3 Trial are clear and immediate. SAPIEN 3 TAVI offers shorter procedure times, fewer days in hospital, lower risk of rehospitalization and immediate improvements in QoL.1–3
Even in a time when hospital resources are constrained, your sAS patients’ are still in urgent need of treatment. They need an option with reliable outcomes and minimal risk, ensuring they spend less time in hospital and get back to their everyday lives sooner. You can guide them to a low-risk treatment by referring them for a TAVI evaluation.
*Kansas City Cardiomyopathy Questionnaire (KCCQ) overall summary scores range from 0 to 100, with higher scores indicating fewer physical limitations and a greater feeling of well-being.2
‡The PARTNER 3 Trial proved that SAPIEN 3 TAVI is superior to surgery with regard to the primary endpoint (all-cause death, all stroke, and rehospitalisation) and multiple pre-specified secondary endpoints.2
Abbreviations:
CI, confidence interval; HR, hazard ratio; KCCQ, Kansas City Cardiomyopathy Questionnaire; sAS, severe aortic stenosis; TAVI, transcatheter aortic valve implantation.
References:
- [1] Mack MJ, Leon MB. Two-year clinical and echocardiographic outcomes from the PARTNER 3 low-risk randomized trial. ACC 2020; Chicago, IL; March 28–30, 2020.
- [2] Mack MJ, Leon MB, Thourani VH, et al. N Engl J Med. 2019;380: 695–1705. Supplementary Appendix included.
- [3] Baron SJ, Magnuson EA, Lu M, et al. J Am Coll Cardiol. 2019;74: 2833–2842.